Deep Brain Stimulation
Neuromodulation Therapy
Deep brain stimulation (DBS) is a surgical treatment that uses an implanted medical device to treat dystonia and other neurological disorders. Once reserved for only severe cases of generalized dystonia, DBS is being used to treat a greater variety of dystonia patients than ever before. The use of DBS is evolving as research progresses. The movement disorders field now has more than two decades of experience and data regarding the long-term safety and efficacy of DBS.
DBS is a neuromodulation technique. Neuromodulation is the process of affecting brain activity to study and treat disease, often by using electrical stimulation.
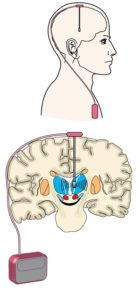
Deep brain stimulation (DBS) is a surgical procedure used to treat a variety of neurological disorders. A battery-powered stimulator —essentially a brain pacemaker—is implanted in the body and delivers electrical stimulation to the areas of the brain responsible for causing dystonia symptoms. The stimulator is implanted in the chest, and extension wires connect the stimulator to leads (electrodes) deep in the brain. In most cases, both sides of the brain are treated. The stimulation to the brain is adjusted by remote control to achieve the appropriate settings for each individual patient.
DBS is completed in several phases:
- Pre-surgical assessment and work-up.
- Implanting the leads deep in the brain.
- Implanting the stimulator in the chest, typically near the collarbone.
- Turning on the stimulator
- Adjusting the stimulation settings
The pre-surgical work-up includes a detailed neurological exam with a movement disorder neurologist. A brain MRI (magnetic resonance imaging) scan may be required. Additional testing may include a neuropsychological evaluation and routine screening to make sure an individual is healthy enough for anesthesia and surgery.
Adult patients are typically awake during the process of implanting the leads, which involves making tiny holes in the skull, and threading the leads deep into the brain. During this process, patients may be asked to respond to questions and instructions from the surgical team in the operating room. More recently, leads can also be implanted inside an MRI scanner with the patient fully asleep. The stimulators and wires are implanted under general anesthesia. After a brief period of healing, the stimulator settings are activated and adjusted over a series of appointments. It can take weeks or months for individuals to achieve full benefit. The stimulator batteries must be periodically replaced by outpatient surgery. Additional programming adjustments may be needed.
Medical centers that offer DBS may vary in their procedures and practices. For example, some centers will implant the leads and stimulators in one day, while others separate those steps by days or weeks. There are different technologies available to precisely map where in the brain the leads are placed. There are several models of stimulator batteries, for example non-rechargeable and rechargeable.
Although deep brain stimulation (DBS) is proven to be a safe and effective treatment for a variety of disorders, the exact mechanism of action is not fully understood. Dystonia occurs when too much signaling from the brain causes abnormal, involuntary muscle contractions and movements. DBS interrupts this abnormal brain activity. The stimulation delivered to the brain by the DBS device weakens the excessive signals and reduces dystonia symptoms.
Deep brain stimulation (DBS) treatment is not appropriate for everyone with dystonia. Not all patients who undergo the procedure will experience the same results. Based on the research to date, individuals who have isolated (primary) dystonia, which means dystonia is the only present neurological disorder, are likely—but not guaranteed—to have the best outcomes from DBS. Patients who are younger, test positive for the DYT1 dystonia gene mutation, and are treated relatively early after symptoms appear may also be more likely to have a good response to treatment. Individuals with cervical dystonia or dystonia acquired by drug exposure (tardive dystonia) may be good candidates for DBS. Individuals with other forms of acquired (secondary) dystonia are evaluated on a case by case basis. There are promising data on the use of DBS to treat myoclonus-dystonia and focal dystonias including cranial dystonias such as blepharospasm and oromandibular dystonia.
Ultimately, DBS may be considered if medications and other treatments are not providing adequate relief, and if the symptoms negatively affect quality of life to the extent that the surgical risks are justified. The first step in the evaluation process for DBS is to meet with a DBS-trained movement disorders neurologist.
The movement disorders field now has more than two decades of experience and data regarding the long-term safety and efficacy of deep brain stimulation (DBS). Overall serious side effects from DBS are rare, but no surgical procedure is without risk. DBS involves making small holes in the skull to implant the leads and surgical incisions to implant the stimulators under the skin near the collarbone. The main risk in DBS is bleeding in the brain during the lead implantation, resulting in stroke. This occurs in about 1% of patients. Infection occurs in approximately 5% of patients. Infection can be serious and warrant the removal of the DBS devices. (If this happens, it may be possible to re-implant the devices once the infection is treated.) Device failure is also a concern, for example wire disconnection or stimulator battery failure. Most complications that occur can be resolved without removing the DBS device.
Once the stimulator is turned on, side effects from stimulation to the brain may include lightheadedness, tingling sensations, speech problems, balance problems, muscle tightness or pain, and new involuntary movements or slowness of movement. Side effects from stimulation can often be lessened or eliminated by adjusting stimulation settings.
In the United States, deep brain stimulation (DBS) for dystonia received a special category of approval by the Food & Drug Administration (FDA), called a Humanitarian Device Exemption. In most cases, insurers cover the procedure. Some insurers may initially deny coverage but approve after an appeal. DBS for dystonia is covered by Medicare and Medicaid.
Deep brain stimulation (DBS) typically requires a one or two night stay in the hospital. In the first days after surgery, there will be temporary swelling of the brain around the implanted leads. This can cause headache, confusion, drowsiness, and sometimes mood changes lasting about a week. There may be incision pain and swelling. Rarely there can be complications with the DBS devices. It may take several weeks for incisions in the head and chest to fully heal. Patients must be diligent in following physician instructions to prevent infection during this time.
The stimulator is typically turned on two to four weeks following surgery, at which point the stimulation settings will be adjusted by remote control. Several appointments, over the course of weeks or months, with a DBS programming expert may be required to determine the ideal settings for the patient’s specific needs. The effects of DBS for dystonia are not immediate. It can take months or a year to achieve full benefit from the therapy.
One of the challenges of treating dystonia with deep brain stimulation (DBS) is that it is difficult to predict which patients will benefit and to what degree. Unlike essential tremor or Parkinson’s disease, the effects of DBS for dystonia are rarely immediate. It can take weeks, months, or even a year to experience the full therapeutic benefit.
From the years of research data available, improvements of 50-60% are generally observed overall, with some patients experiencing a 90% reduction in symptoms and disability. Depending on the individual patient, however, even an improvement rating of 30% can have a significant positive impact on a person’s ability to function. It is not uncommon for DBS patients to rate their improvement higher than the numerical rating scales that doctors use to measure symptom severity and disability.
In a review of DBS in children (under 21 years), outcomes from DBS were compared among different types of dystonia. The review reported that children with inherited dystonias without any structural damage to the brain experience a median 76% improvement of movement symptoms and disability. Children with inherited dystonia disorders associated with structural changes to the brain experienced a median improvement of 27%. Children with dystonia and cerebral palsy or other acquired dystonias demonstrated 10% improvement. Children with isolated (primary) dystonia of unknown causes (i.e. no identified genetic mutation) experienced a median improvement of 50%.
The expected life span of a deep brain stimulation (DBS) battery at a typical voltage is about four years. At a very high voltage, the battery may need to be replaced after a year; at a very low voltage, perhaps up to seven years. Replacing a battery can be done under general or local anesthesia as an outpatient procedure. Rechargeable batteries are now available, and DBS technology is evolving quickly with a focus on innovations to strengthen battery performance and reduce the need for battery replacements.
Having deep brain stimulation (DBS) is a life-long commitment that requires ongoing management. Maintenance may include battery changes (which consist of outpatient surgery) and ongoing adjustments to the stimulation settings. Device problems may occur. The most common device problem is lead breakage, which is reported in about 4% of cases, but this occurs less frequently with newer devices. Rarely, individuals develop new movement disorder symptoms associated with the neurostimulation. Individuals with DBS must be mindful of situations that can interfere with the functioning of the DBS devices. This includes certain medical MRI imaging (magnetic resonance imaging), diathermy therapies (shortwave, microwave, and ultrasound), security metal detectors, and security wands. There may be restrictions on certain activities, such as contact sports that could damage the implanted medical devices. Individuals with DBS carry a medical device card that indicates they have an implanted medical device and provides safety information from the manufacturer and physician contact information. Some individuals chose to wear a medical alert bracelet or necklace indicating they have an implanted medical device.
Individuals who may be candidates for deep brain stimulation (DBS) undergo careful examination to ensure the procedure is appropriate for them. This includes an extensive neurological evaluation. A neuropsychological evaluation is needed to observe how the brain is functioning cognitively, mentally, and emotionally. A neuropsychological assessment will identify any problems that could prevent DBS from being an appropriate choice for that patient. For example, certain conditions, such as dementia or severe depression, may prevent someone from being a good candidate for DBS. The neuropsychological assessment also provides a baseline before surgery, so that any changes in cognitive or mental functioning that may occur after surgery can be readily identified and investigated.
The neurological evaluation is not a test that a patient “passes” or “fails.” It is a series of exercises to understand how the brain is functioning. The evaluation is typically conducted one-on-one with a neuropsychologist and can take several hours to complete. The exam includes an interview and written or typed questionnaires.
Neurosurgical teams that offer deep brain stimulation (DBS) will have specific recommendations about the extent to which a patient’s scalp must be shaved before surgery. Some surgical teams recognize that individuals can feel apprehensive about removing their hair and take measures to minimize the shaved area. In some cases, shaving the head is critical to incision hygiene and preventing infection, which can be a serious and challenging complication.
Neurosurgical teams that offer deep brain stimulation (DBS) will have specific recommendations about whether adults are required to be awake for the part of the procedure in which the leads are put in place. It depends to a large degree on the comfort of the patient and preference of the surgical team. Children are typically under general anesthesia during lead implantation and battery implantation.
Deep brain stimulation (DBS) for dystonia is a highly specialized procedure that should be performed by a team of medical experts with extensive training and experience. Each medical center that offers DBS will have its own methods and procedures. The first step in the evaluation process for DBS is to meet with a DBS-trained movement disorder neurologist. The DMRF can help locate movement disorder centers in your region.
If you are considering DBS or if DBS has been recommended to you by a movement disorder specialist, consider discussing the following questions with your doctors:
- Am I a good candidate for DBS, and why?
- What are the steps of the DBS process?
- Tell me about the brand and model of DBS device recommended for me and how it works.
- What are the advantages of having DBS?
- What benefits can I expect?
- What are the risks during surgery, after surgery, and long-term?
- What happens if I don’t have DBS? Is there an alternative treatment plan?
- What is the experience of the medical center and surgical team with DBS for dystonia?
- Does the medical team publish the outcomes of their DBS program?
- What is the most common complication your DBS patients have and how are they resolved?
- What percent of your DBS patients develop infection?
- Where will the surgeries be done?
- Who will program my DBS stimulator, and what is their experience with dystonia?
- Where will the stimulator adjustments take place? How many appointments, over what period of time, should I expect?
- What kind of anesthesia will be used? Will I be awake for parts of the procedure?
- How long is the recovery?
- What rehabilitation/physical therapy is necessary?
- What will my scars look like?
- Will DBS reduce the need for oral medications or botulinum neurotoxin injections?
- Where can I get a second opinion?
- How much does DBS cost and who will pay for it?
- Is there anything about DBS I should know that we have not yet discussed?
The first step in the evaluation process for DBS is to meet with a DBS-trained movement disorders neurologist. The DMRF can help you locate centers in your region.
Additional resources include:
Surgical Interventions for Dystonia

DBS Patient Perspective

Brain Sensing & Adaptive DBS